Welcome to my channel, Chaz’s Lifestyle! In todays video, we’re creating simple, affordable & easy meal preps! Come hang out …
source
MEAL PREPS FOR WEIGHT LOSS|| I LOST 17 lbs In 2 Weeks: Meal Prep Ideas
Baby Food || weight gain & Healthy
Hello everyone! Thank you for watching our videos.
Facebook : https://www.facebook.com/priyavantalu1
Instagram: https://www.instagram.com/vantalupriya/
source
10 Fruits that are great for PCOS 🍒 #pcos
Follow my channel @PCOSWeightLoss for more tips on PCOS friendly foods, recipes, workouts, and how to lose weight with PCOS!
source
My Korean Head Spa experience
Sharing the details on my Korean head spa experience and why it’s worth booking a trip to Korea just for this (but also stay for the amazing culture, food, and people!).
Hi friends! How are ya? I hope you’re having a lovely morning so far. We’re officially back in the swing of life over here. I subbed a barre class yesterday, and we have a mold remediation appointment today. Now that we’re back in town, it’s time to tackle that beast.
But for now, let’s talk about relaxation and spa-y things… like my amazing Korean head spa experience.
Here are all of my Korea and Japan posts in one spot – I’ll be adding links as they go live!
Seoul recap, what we did and what we ate
Tokyo and Kyoto itinerary and tips for travel
What we ate in Japan
My Korean Head Spa experience (this post)
When we decided we’d be visiting Korea, I knew I wanted to take advantage of some skin or beauty treatments. While it would’ve been easy to go WILD, I didn’t want to miss out on adventures with the fam. I figured a head spa appointment would be perfect because it would only take an hour or so, there were tons of locations close to our hotel, and they all had amazing reviews.
I booked a last-minute appointment at Hair the Beau and had no clue what to expect.
When I walked in, the main stylist, Raon, introduced herself and helped me get set up with a locker. Then I was led to a sitting area to have my scalp scanned.

I won’t post the before picture here, but let’s just say my scalp was kind of horrendous. Leading up to this appointment, I would only wash my hair once a week. My hair can get really dry, and I felt like washing it less helped prevent dryness. My hair didn’t get greasy, and it can hold a curl or style for a long time, so I didn’t really see a need to wash it more often. I thought it was better for me?
Turns out, the base of my hair follicles had tons of buildup from grime and dead skin. I literally felt ILL when she scanned my scalp and the image was projected onto a tiny screen in real time.
She recommended the full treatment for me and said it would take about two hours. I told her I only had an hour or so, and she said they could finish everything in an hour and 15 minutes, which worked for me. (The Pilot and the kiddos were off to a petting zoo, so I figured they’d be entertained for a bit.)
She also explained that my hair would cost extra because it was so long. I had no clue what I was getting myself into, but I decided to trust the process and the amazing reviews I’d read online.
My Korean Head Spa experience
Hair the Beau Hongdae
The full treatment:


She sat me down and another stylist came over, and they started brushing my hair. After it was fully brushed, they added an elixir to my entire scalp, scrubbed it in, and put a bubbler machine over my head for five minutes. I’m not exactly sure what the bubbler machine did, but I can assure you that Korea is living in the future.
After that, it was time to head to a separate room, which is where the majority of the treatment took place. The shampoo bowl had a chair that was also a full-body massager, and it felt heavenly.


She started working on my hair and honestly, I pretty much transcended during this portion of the experience. She washed my hair maybe six times, added a mask, more elixirs, a peptide treatment, a cool waterfall rinse situation, and then massaged my head and shoulders for what felt like 20 minutes. It was pure bliss. The scalp massage is usually my favorite part of a massage anyway, so this was next-level.
After the treatment, they led me to a styling chair and rescanned my scalp. I couldn’t believe the difference. It looked so clean and healthy.

Then they did a tandem blow dry and straighten on my hair,


and my hair felt the best it’s ever felt in my entire life.
This is a screenshot from IG with a filter but you can see how sleek and shiny it was!


She also shared the products she recommended for maintaining my results at home, and I ended up buying the shampoo, mask, hair milk, and elixir.
Here were the recommended at-home steps:
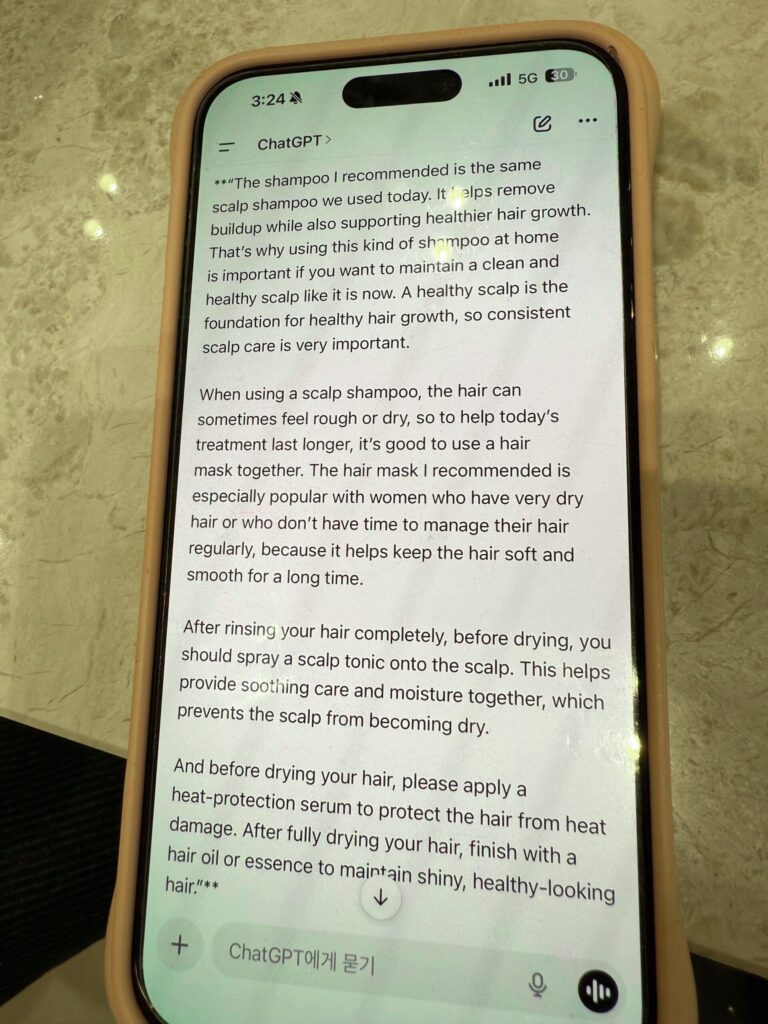

I also linked everything I could find online in this collection!
The grand total was about $375 for the treatment and products. In the States, the treatment alone probably would’ve been closer to $500. If you find yourself in Seoul, I highly, highly recommend seeking out a head spa treatment. I’ve also heard amazing things about skincare, lasers, body adjustments, and traditional medicine treatments in Seoul.
Have you ever done anything like this before? If you’ve done it in the States, how much did it cost??
A friend recommended a scalp facialist here in Tucson, so if I end up doing it again locally, it’ll be interesting to compare.
Have a lovely day, and I’ll see ya tomorrow with a giveaway!
xo
Gina
Giant Chicken Milanese (Viral Sheet Pan Chicken Cutlet)
This Giant Chicken Milanese is a crispy baked ground chicken cutlet topped with a fresh lemony arugula salad.

Viral Ground Chicken Cutlet
Chicken Milanese is one of my favorite dishes to order when I go out for Italian, so I knew I had to try the viral giant chicken cutlet from Skyler Bouchard. Instead of the traditional pounding and deep-frying, we press seasoned ground chicken into a single large cutlet, coat it with panko, and bake it on a sheet pan until golden and crispy, ready to slice and share. I topped mine with lots of baby arugula, shaved parm and fresh lemon juice, my favorite way to enjoy it! More lighter versions of Chicken Milanese using chicken breast in the air fryer, try my Air Fryer Chicken Milanese with Baby Arugula and my Chicken Milanese with Mediterranean Salad, both delicious!
Ingredients You’ll Need
Here’s everything you need to make this easy ground chicken Milanese. See the recipe card below for the exact measurements.

- Ground Chicken: Classic Milanese uses chicken breasts, but for this sheet pan cutlet, we’re using 93% lean ground chicken.
- Seasoning: Garlic powder, onion powder, kosher salt
- Parmesan: Grated Parm for the meat mixture and shaved for the arugula salad
- All-purpose flour prevents the chicken from sticking to the parchment paper.
- Eggs help the panko stick to the chicken.
- Seasoned Panko: We’re using panko to coat the chicken, which will give it a crispy crust.
- Olive oil spray helps the panko get crispy in the oven.
- Arugula has a peppery flavor.
- Vegetables: For a summer twist, add cherry tomatoes and corn to the salad.
- Olive oil and lemon juice create a simple vinaigrette.
How to Make Ground Chicken Cutlet
If you don’t want to flip the sheet pan chicken cutlet, you can skip breading the other side, which is also great if you want to reduce carbs and calories. See the recipe card at the bottom for printable directions.



- Season the ground chicken with garlic powder, onion powder, salt, and grated Parmesan.
- Make the giant cutlet: Sprinkle a parchment-lined sheet pan with flour, then press the chicken into a disc shape. Sprinkle the top with the remaining flour and cover with parchment. Flatten the chicken with a rolling pin until it’s a quarter-inch thick.
- Add the panko: Brush the chicken with the whisked eggs and sprinkle with panko. Press to ensure they stick.
- Flip the cutlet: Spray another baking sheet with olive oil, then flip the cutlet onto it. Coat with the remaining egg and panko, then spray with olive oil. The more you spray, the crispier it’ll get.
- Bake the chicken cutlet at 400°F for 25 to 30 minutes. Then, increase the heat to 425°F and bake for an additional 5 minutes.
- Top with arugula: Baby arugula, shaved Parmesan and fresh lemon juice is perfect here!


Customize It
- Ground Chicken: Substitute ground turkey.
- Make it gluten-free: Use GF flour and panko.
- No seasoned panko? You can use plain panko or add dried herbs like parsley or oregano to the mix.
- Dairy-free: Skip the Parmesan.
- Salad options: Swap arugula with baby spinach or mixed greens.
Serving Suggestions
I love this giant ground chicken cutlet topped with arugula salad, but you can also en with another side dish.
Storage
- Refrigerate the chicken for 4 days. The salad with dressing won’t hold, so it’s best to make only what you plan to eat that day.
- Freeze for up to 3 months.
- Reheat: Microwaving the breaded cutlet will make it soggy, so it’s better to reheat it in the air fryer, oven, or skillet. Air fry or bake the chicken at 350°F for 5 to 10 minutes, or warm it up on the stove over medium heat.

More Ground Chicken Recipes You’ll Love
For more dinner inspiration, check out these five healthy ground chicken recipes!

Yield: servings
Serving Size: 1 /4 of the cutlet and salad
-
Preheat oven to 400°F.
-
In a medium bowl combine ground chicken, garlic powder, onion powder, salt and ¼ cup of grated parmesan. Reserve.
-
Line a baking sheet with parchment paper and sprinkle with 2 tablespoons of flour; place chicken in the center and slightly press into a disc shape (I did this on the counter). Sprinkle the top with the remaining 2 tablespoons of flour and cover with an additional piece of parchment paper.
-
Use a rolling pin to roll the chicken into a giant cutlet, about ¼” thick.
-
Gently remove the top layer of parchment (if any chicken sticks to the parchment, take it off and press it back on to the top of the cutlet).
-
Brush the top of the cutlet with ½ of the whisked egg (1 egg per side). Sprinkle the cutlet with ¾ cup of panko breadcrumb and press the crumbs in well so they don’t move out of place.
-
Prepare an additional baking sheet with olive oil spray* and flip the cutlet, breaded side down, onto the sheet.
-
Repeat the egg and panko step with the top of the cutlet and then spray with more cooking spray. Bake, 25-30 minutes until you can pick the bottom of the cutlet up and see it becoming a golden brown. Raise the oven to 425°F and cook for an additional 5 minutes.
-
While the cutlet is cooking, prepare the salad: In a medium bowl, combine arugula and remaining 2 tablespoons shaved parmesan with 1 tablespoon olive oil and lemon juice. Reserve.
-
Serve giant chicken cutlet with arugula and shaved parm on top and lots of lemon juice
Last Step:
Please leave a rating and comment letting us know how you liked this recipe! This helps our business to thrive and continue providing free, high-quality recipes for you.
If you have a hard time flipping, you can bread one side and leave the other side on the parchment and bake with half the crumbs.
Serving: 1 /4 of the cutlet and salad, Calories: 317.5 kcal, Carbohydrates: 21 g, Protein: 31 g, Fat: 12.5 g, Saturated Fat: 4 g, Cholesterol: 185.5 mg, Sodium: 820.5 mg, Fiber: 1.5 g, Sugar: 1 g
A Persistent Pesticide Is Linked to Alzheimer’s Risk
How can we avoid the breakdown products of pesticides that may increase the risk of Alzheimer’s disease as much as if you carried APOE e4, the so-called Alzheimer’s gene?
Although there is a growing list of Alzheimer’s disease susceptibility genes, those genes account for less than half of all Alzheimer’s cases. Here is the “single most compelling” piece of data on the potential control we have over the disease: When it comes to identical twins with the exact same genes, if one gets Alzheimer’s, the other usually does not. So, we have to think about all the other contributing factors beyond just genetics.
There’s a list of chlorinated pesticides, including DDE (a metabolite of DDT), that the U.S. Environmental Protection Agency has classified as probable human carcinogens. But in a study—which I’ve mentioned in a video on pesticides and cancer—blood levels of DDE and other pesticides were associated not with increased cancer mortality, but increased risk of other-cause mortality. This led researchers to speculate that this may be due to an associated increased risk of diabetes or dementia. I’ve talked previously about the diabetes link. What about dementia?
A research team at Rutgers found significantly higher blood levels of DDE in Alzheimer’s disease patients compared to controls, as you can see below and at 1:22 in my video Pesticides (DDT) and Alzheimer’s Disease.
Autopsy studies show blood levels are a good proxy for brain levels. Those patients with the highest levels were at about four times the odds of having dementia from Alzheimer’s. And in a petri dish, DDE increases amyloid precursor protein levels in human brain cells, providing a potential mechanism. Below and at 1:48 in my video, you can see the levels of the sticky protein implicated in the development of Alzheimer’s disease before and after DDE is added at the levels one finds circulating in highly exposed individuals among the general population.
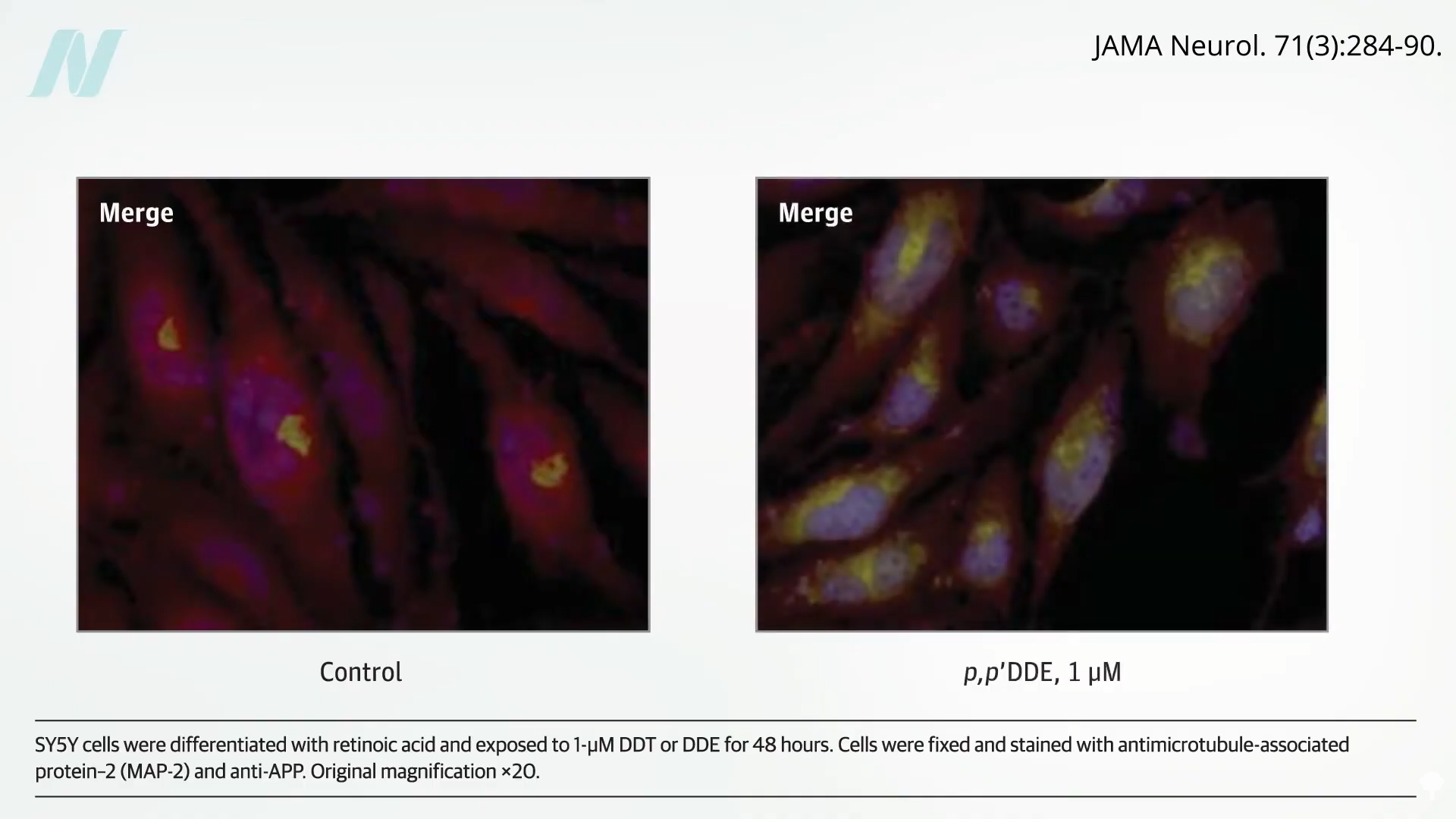
Put all these studies together, and there does indeed seem to be a link, consistent with data showing about a doubling of risk for developing dementia among those acutely pesticide-poisoned, as you can see below and at 2:01 in my video.
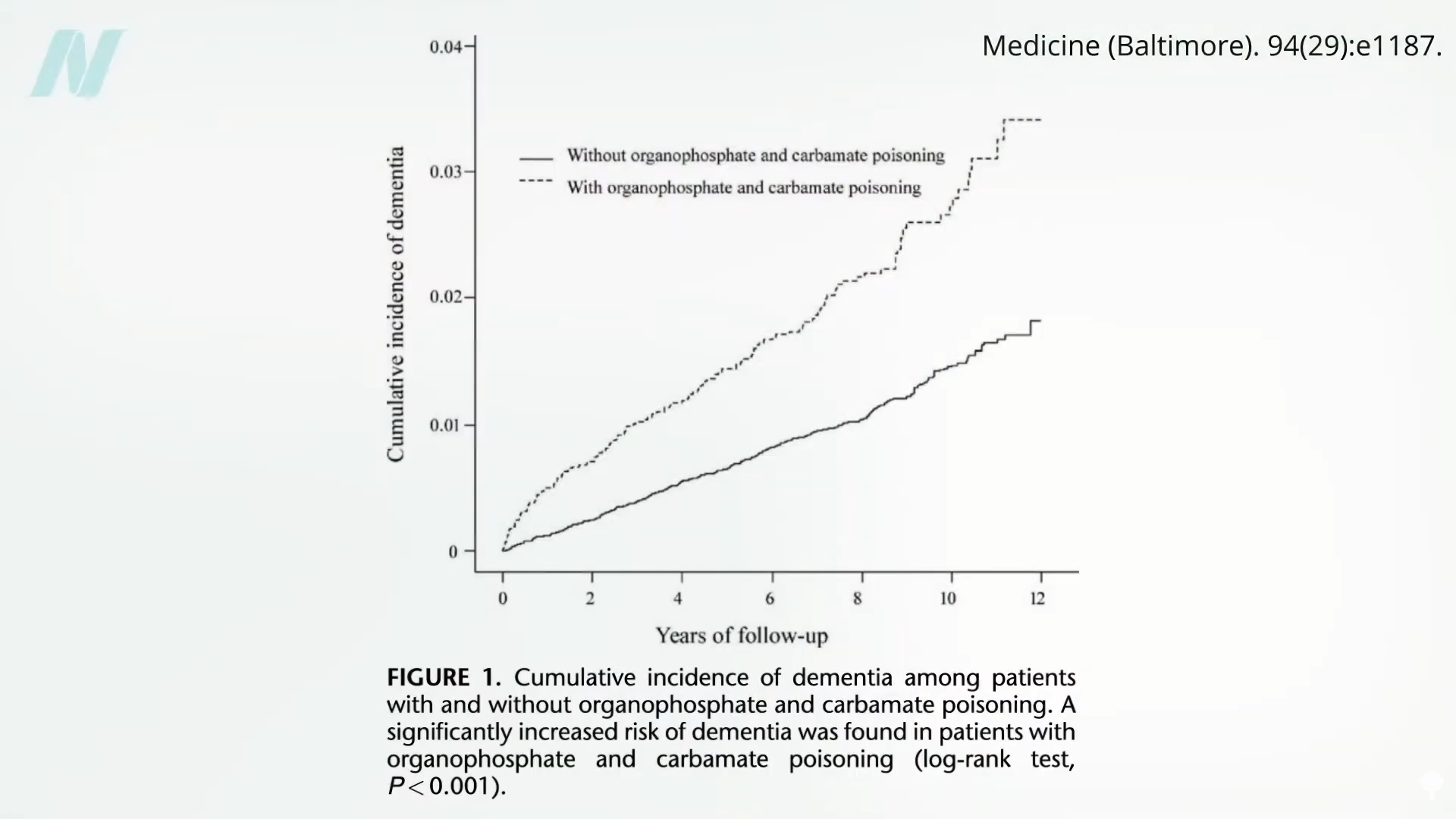
Among U.S. elders, DDT and its breakdown product DDE are also associated with increased risk of cognitive decline in general, which is shown below and at 2:08 in my video.
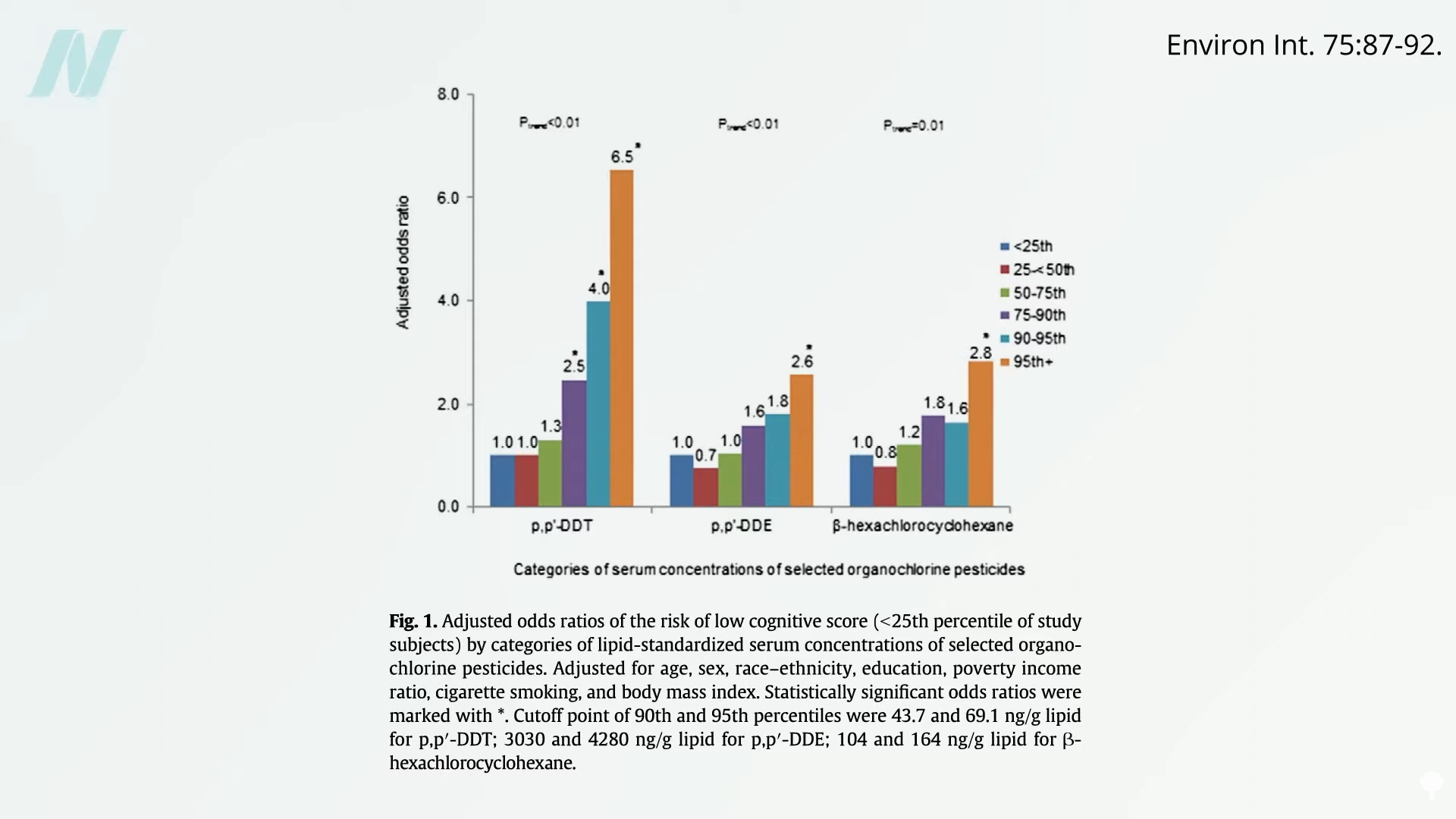
DDT was used extensively in the United States from the 1940s through the early 1970s. At its peak, we were churning out about 180 million pounds a year. And it is still in our bodies to this day, contaminating the bloodstreams of more than 90% of Americans, with DDE—the pesticide linked to quadrupling the odds of Alzheimer’s—found at the highest levels of all.
It’s still in our bodies because it’s still in the food supply. In a previous video on the topic, I noted that the levels of DDT, DDE, and other banned pesticides and pollutants were much lower in the breast milk from a vegetarian mother compared to breast milk of her non-vegetarian sister. The largest difference was noted for DDE, which was four times lower in the vegetarian sister. This is what you see across the board for these kinds of pollutants. Below and at 3:20 in my video, you can see the levels of dioxins and PCBs found in beef, chicken, pork, processed meat, eggs, fish, dairy products, and all plant foods put together when food samples were collected from supermarkets across the United States.
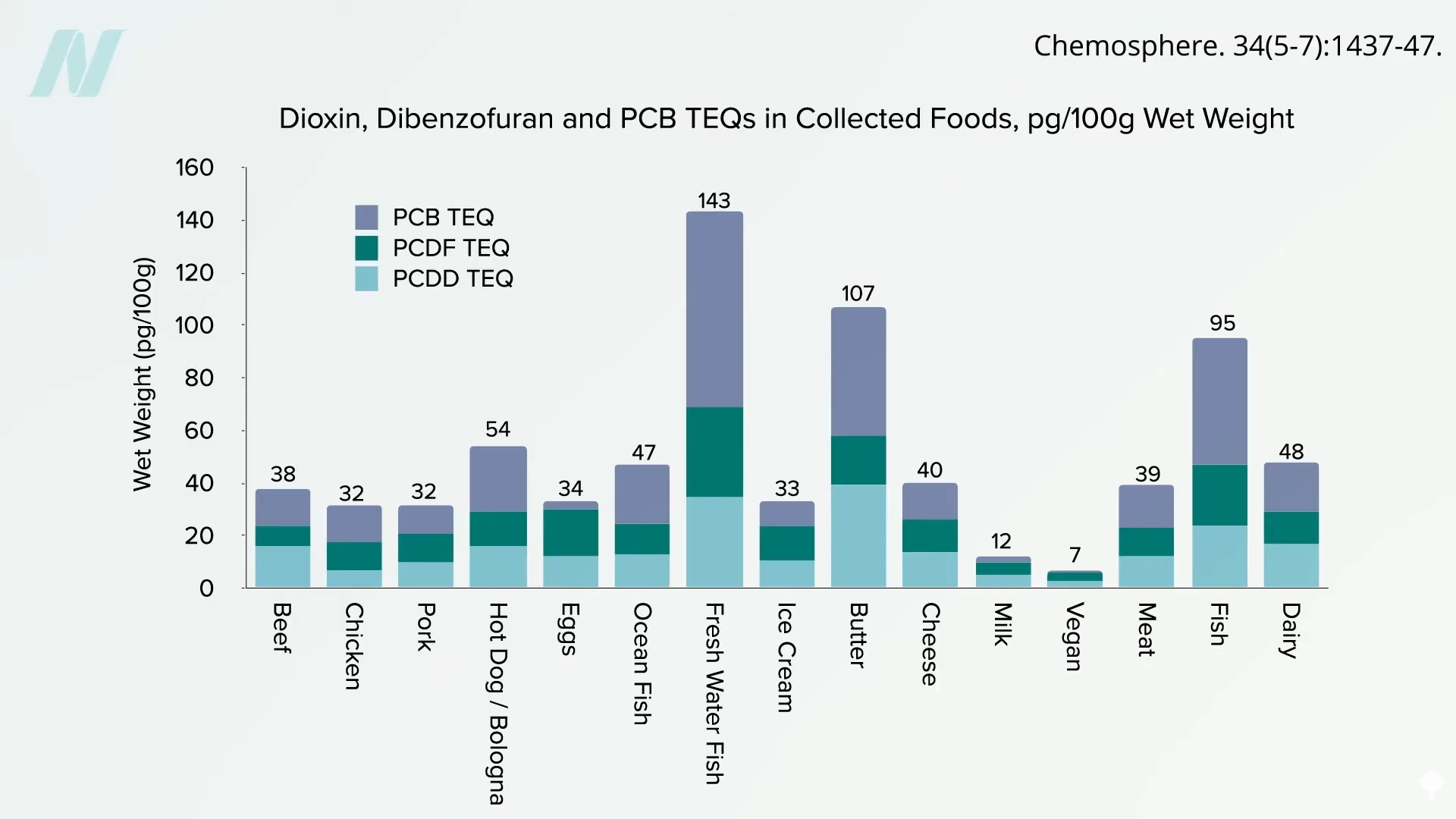
These toxins build up in the food chain, so it makes sense that the most contaminated foods are meat, fish, and dairy products. The toxin levels were found to be 5 to 10 times higher in meat, eggs, fish, and dairy compared to plant foods. Unfortunately, cooking doesn’t destroy pollutants like DDE—in fact, it may make them even more concentrated. And this is for a pesticide that may increase the risk of Alzheimer’s disease as much as if you carried the so-called Alzheimer’s gene APOE e4.
Doctor’s Note
The video I mentioned is Pesticides and Cancer Risk.
For more videos on Alzheimer’s disease, check out the Alzheimer’s topic page.
High protein, low carb, low calorie, keto breakfast meal prep! #mealprep #healthybreakfast #eggs
🔗RECIPE is in on my blog mattsfitchef.com + https://mattsfitchef.com/breakfast-casserole/
📍OR search “Breakfast Casserole” in the search bar on my website https://mattsfitchef.com
source